Many couples focus only on ovulation and sperm quality during fertility treatment. However, one crucial factor often gets ignored — endometrial receptivity.
This factor directly affects implantation. Even if fertilization occurs successfully, pregnancy cannot happen without a receptive uterine lining.
Therefore, understanding the role of endometrial receptivity and IUI success can help improve your chances and guide better treatment decisions.
What is Endometrial Receptivity in Fertility Treatment?
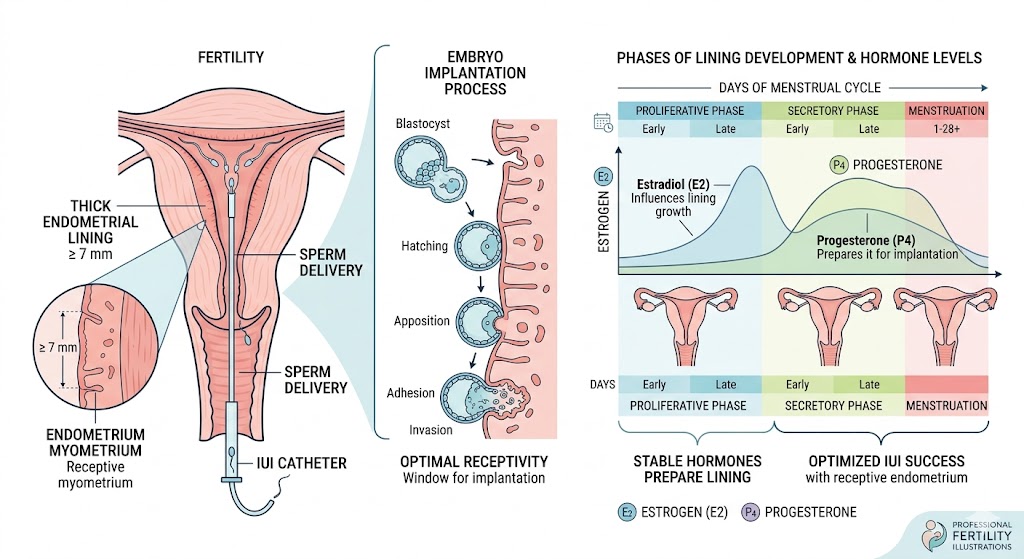
Endometrial receptivity refers to the short period when the uterine lining becomes ready for embryo implantation.
During each menstrual cycle, estrogen helps the lining grow and thicken. After ovulation, progesterone prepares the lining for implantation.
This creates a specific time frame called the window of implantation.
If the embryo reaches the uterus during this window, implantation becomes more likely. However, if the timing does not match, implantation may fail.
Why Endometrial Receptivity Matters for IUI Success
In IUI, fertilization takes place inside the body. However, implantation depends entirely on the condition of the uterine lining.
If the lining is not properly prepared:
- The embryo may not attach
- Pregnancy may not occur
- The cycle may fail
Therefore, endometrial receptivity becomes as important as sperm quality and ovulation timing.
Ignoring this factor can lead to repeated unsuccessful cycles.
Key Factors That Affect Endometrial Receptivity
Several medical and lifestyle factors influence the receptivity of the uterus.
Hormonal Balance
Estrogen builds the lining, while progesterone makes it receptive. Any imbalance can disrupt implantation.
Ovulation Timing
Precise timing ensures that fertilization and implantation occur in sync.
Blood Flow
Healthy blood flow supports proper growth of the uterine lining.
Age and Health Conditions
Age, thyroid disorders, and PCOS can affect uterine readiness.
Because these factors work together, even a small issue can reduce IUI success.
Ideal Endometrial Thickness for Better IUI Outcomes
Doctors usually evaluate the uterine lining using ultrasound.
An endometrial thickness of 7–8 mm or more is generally considered favorable for implantation.
Additionally, a trilaminar pattern (three-layer appearance) is often associated with better outcomes.
However, thickness alone does not guarantee success. Many patients with thinner lining may still conceive, while others may need additional support.
Common Uterine Conditions That Reduce Implantation
Certain uterine conditions can reduce endometrial receptivity and lead to failed cycles.
Fibroids and Polyps
These growths may interfere with embryo attachment.
Chronic Endometritis
A mild infection can affect the uterine environment.
Adhesions
Scar tissue inside the uterus may disturb implantation.
Hormonal Disorders
Conditions like thyroid imbalance can affect the lining.
Early diagnosis and treatment of these conditions can improve fertility outcomes.
How Doctors Assess Endometrial Receptivity?
Doctors use simple and effective methods to evaluate receptivity.
- Ultrasound to check thickness and structure
- Monitoring hormone levels
- Tracking ovulation timing
In most cases, these methods provide enough information to plan treatment. Advanced tests are used only in selected situations.
Ways to Improve Endometrial Receptivity
Improving receptivity requires a combination of medical support and lifestyle care.
Medical Treatment
Doctors may prescribe estrogen or progesterone supplements to support the lining.
Lifestyle Changes
Good sleep, stress control, and a balanced diet support fertility health.
Treat Underlying Problems
Removing fibroids or treating infections improves the uterine environment.
Follow Proper Timing
Taking medications at the right time ensures better synchronization.
Even small improvements can increase the chances of implantation.
Endometrial Receptivity and Failed IUI Cycles
Repeated IUI failure is not always related to egg or sperm quality.
In many cases, poor uterine receptivity becomes the hidden cause.
If multiple cycles fail, doctors usually reassess:
- Endometrial thickness
- Hormonal balance
- Timing of insemination
Addressing these factors can improve future treatment success.
When to Consult a Fertility Specialist?
If you experience repeated IUI failures or irregular cycles, expert advice becomes important.
Consulting an infertility specialist in Noida can help identify the exact cause and guide the right treatment plan.
If advanced treatment is required, visiting a trusted IVF center in Noida can provide better options and improved success rates.
Timely consultation can prevent delays and improve outcomes.
Expert Fertility Care in Noida – Dr. Aprajita Srivastava
Dr. Aprajita Srivastava is a highly skilled gynecologist, IVF specialist, and laparoscopic surgeon based in Sector 121, Noida. She has extensive experience in reproductive medicine and infertility treatment.
She specializes in advanced procedures such as IUI, IVF, and fertility preservation. Her approach focuses on identifying root causes and providing personalized treatment plans.
Patients looking for comprehensive reproductive care often consult her as the best gynecologist in Noida for accurate diagnosis and effective care.
With her expertise and patient-centered approach, she helps couples move forward with confidence and improved chances of pregnancy.
Dr. Aprajita Srivastava is a highly experienced IVF Specialist in Noida, Gynecologist, and Obstetrician with over 13 years of expertise. Holding an MBBS, DGO, and a Fellowship in Minimal Access Gynaecology Surgery & Reproductive Medicine, she specializes in IVF, IUI, and advanced fertility treatments.
Practicing at Qure Clinic, Sector 121, Noida, Dr. Aprajita is dedicated to compassionate care, personalized solutions, and helping families achieve their dream of parenthood.

